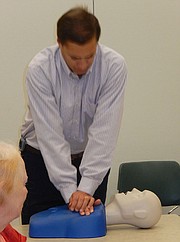
Demonstrating CPR, EMT/paramedic Gary Orski locks his arms and uses his upper-body strength and abdominal muscles to compress this mannequin’s chest. Photo by Bonnie Hobbs.
No one knows if or when he or she will be in a position to save a life. But to prepare for such an event, state-certified EMT/paramedic Gary Orski gave lessons to local residents.
A volunteer EMT with the Prince William County Fire Department, he spoke at a recent meeting of the Sully District Police Station’s Citizens Advisory Committee. As he did so, he also demonstrated the techniques on mannequins.
“The job of an EMT/paramedic is to provide quality, emergency care and improve the health of the communities we serve,” said Orski. He then showed those attending how to perform CPR and also referred them to the American Heart Association’s website, www.heart.org, for further information.
First, he said, make sure the scene is safe. “Shake the victim and shout, ‘Are you all right?’” said Orski. “If there’s no response, call 911 and, if possible, get an AED (automated external defibrillator) and a first-aid kit. Run your hand above the person’s nose to check for breathing, for about 10 seconds — and count out loud. If there’s no breathing, start CPR. Don’t check for a pulse unless you’re trained to do that.”
Then, he said, “Make sure the patient is on their back and anatomically locate their heart in the center of their chest. Push hard, fast and deep, at least 2 inches — and for an adult, as hard as you can. Push at a rate of about 100-120 beats per minute.”
When someone is unconscious and not breathing, said Orski, “The premise is that their heart has stopped. So we try to save their lives. By just doing compressions on their chest, you’ll circulate their blood and keep them alive. And that will hopefully jumpstart them until help arrives.”
Using the mannequin to illustrate, he then locked his arms and used his upper-body strength and abdominal muscles to compress the chest with both hands. He also noted that doing so to the tune of the song, “Stayin’ Alive,” would ensure the proper rate of pushing.
Orski said the patient’s head should be tilted back, with the chin lifted. “Place the palm of your hand on their forehead,” he said. “Place the fingers of your other hand under their jaw, but do not press on the tissue underneath the jaw.”
Then, he said, “Gently extend the head and neck to open the airway. Look in the patient’s mouth for obstructions and remove any you see. Do not do a blind, finger sweep. If it’s a stranger, you can just do chest compressions. But for people you know, combine compressions with breaths.”
Orski said 30 compressions followed by two breaths equals one CPR cycle, and five cycles of CPR equals 2 minutes of CPR. “Everyone gets tired after doing five cycles,” he said. “So if another person is there to help, switch with them then.”
And if an AED is handy, so much the better. Said Orski: “Using an AED within the first minute immediately following CPR improves a patient’s survivability to 90 percent.”
Instructing attendees how to use an AED, he said people should turn it on and follow its audio prompts, “The heart starts to quiver or fibrillate, but using the AED stops that,” said Orski. “Its electrical shock stops the chaos.”
So, he explained, “Turn on the AED and put the pads on the patient’s bare chest — on their upper right and lower left sides. Connect the electrodes and press the ‘analyze’ button.”
“Make sure no one touches the patient while the AED analyzes the heart,” he continued. “Then stand clear of the patient when hitting the button to deliver the AED’s electrical energy to the heart.”
After two minutes, the AED will re-analyze the situation. If the AED says, “No shock required,” said Orski, “It means the heart has flatlined and has no fibrillation to stop, so you have to do CPR.”
He then instructed people what to do if an infant or child stops breathing. “For toddlers and preschoolers under 45 pounds and under 5 years old, just use one arm and only go one-third of their depth with the compressions,” he said.
For babies, said Orski, “Use just two fingers and go one-third of the depth between their anterior and posterior planes. Because babies are very flexible, you’re not going to break their bones. But the 30 compressions, the rhythm and the five cycles are the same as with adults. You’re pumping the heart and circulating the blood.”
Next, he discussed first aid for choking victims. With a choking adult, said Orski, “Do an abdominal thrust. Stand behind them and make a fist with your dominant hand, with your thumb touching your ring finger. Put your leg between theirs, put your fist above their belly button and thrust up and in.”
If the person is too tall, he said, “Have them kneel or sit down. Or if they’re too big, place them against a wall and press on their chest with two hands and your head down. For a pregnant mom in her second or third trimester, make a fist under her sternum and press straight back.”
In the case of a child who, for example, has inhaled food down his or her windpipe, first verify what’s happened. “To see if a preschooler or toddler is choking — because they don’t know how to tell you — ask them their name,” said Orski. “And if they can’t answer, they’re choking and need help, so do an abdominal thrust. But kneel down and align your shoulders with theirs, and use one arm, instead of two.”
For babies, he said, “Sit down, put your legs together and put the baby on them, head down. Do five back slaps and five chest compressions.”
Orski said people may never be called upon to use any of these lifesaving techniques. But, he added, “As a community, the more of us that can step up and help someone else when they need it, the better.”